Reducing unnecessary surgeries: New tech identifies lesions most likely to develop into breast cancer
10/22/2017 / By Jhoanna Robinson
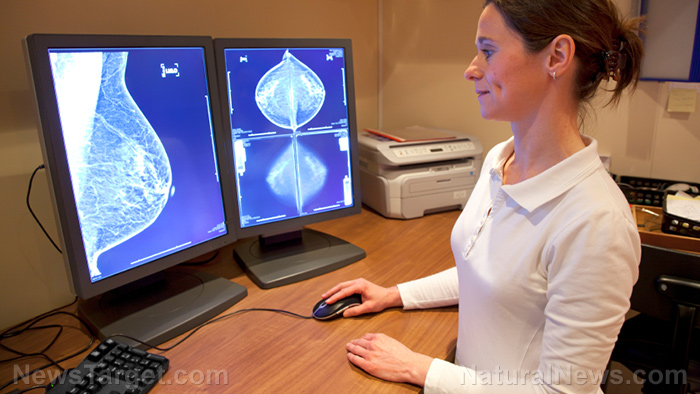
Thousands of women each year subject themselves to painful and invasive surgeries to get rid of breast lesions which turn out to be benign, defeating the purpose of the surgeries in the first place. To avoid occurrences of these unnecessary surgeries, scientists are working on making current detection and diagnostic tools more effective and accurate.
A new study that was published in the online journal Radiology features a machine learning tool that can tell if a high-risk breast lesion can become cancerous, paving the way for the reduction of unnecessary surgeries.
Mammograms are still the best detection tool for finding out whether a woman has breast cancer. Lesions that are detected are then tested using a needle biopsy. If the biopsy is found to be abnormal, a patient will have to undergo surgery to remove the lesion.
At present, doctors opt to remove breast lesions even if they are not sure whether they can cause cancer or not, since the existence of breast lesions in a woman’s body is indicative of a greater risk of cancer development. With this new technology, patients can opt to be safely monitored instead of undergoing life-risking surgery, sparing them thousands of dollars and costs and a whole slew of health complications.
“There are different types of high-risk lesions. Most institutions recommend surgical excision for high-risk lesions such as atypical ductal hyperplasia, for which the risk of upgrade to cancer is about 20 percent. For other types of high-risk lesions, the risk of upgrade varies quite a bit in the literature, and patient management, including the decision about whether to remove or survey the lesion, varies across the practices,” said study author and radiologist Manisha Bahl, M.D., M.P.H., from Massachusetts General Hospital (MGH) and Harvard Medical School, which are both in Boston.
Dr. Bahl and his colleagues from MGH conducted the study in collaboration with researchers from the Massachusetts Institute of Technology’s Computer Science and Artificial Intelligence Laboratory (CSAIL) in Cambridge, and breast imaging experts at MGH.
“Because diagnostic tools are inexact, there is an understandable tendency for doctors to over-screen for breast cancer. When there’s this much uncertainty in data, machine learning is exactly the tool that we need to improve detection and prevent overtreatment,” said co-author and MIT electrical engineering and computer science professor Regina Barzilay, Ph.D.
Machine learning is a kind of artificial intelligence in which a prototype imbibes intelligence and improves on it based on past experiences, similar to the way that humans gain knowledge. The model that the researchers created studied conventional risk factors like patient age and lesion histology, along with other unique features, including words that appear in the text from the biopsy pathology report.
The researchers trained the prototype to conduct an examination on a group of patients with biopsy-proven high-risk lesions who had already undergone surgical procedures or at least a two-year imaging follow-up. The machine indicated that 115 cases or 11 percent of the 1,006 high-risk breast lesions have the ability to become cancerous.
Researchers tested the machine learning model on the remaining 335 lesions – it correctly predicted that 37 or 38 lesions, or 97 percent, can be upgraded to cancer. They concluded that with the use of this tool, one-third of benign and unnecessary surgical procedures can be avoided.
“Our study provides ‘proof of concept’ that machine learning can not only decrease unnecessary surgery by nearly one-third in this scientific patient population, but also can support more targeted, personalized approaches to patient care,” said Harvard Medical School professor, MGH breast imaging director, and study senior author Constance Lehman, M.D., Ph.D.
“In the past we might have recommended that all high-risk lesions be surgically excised. But now, if the model determines that the lesion has a very low chance of being cancerous in a specific patient, we can have a more informed discussion with our patient about her options. It may be reasonable for some patients to have their lesions followed with imaging rather than surgically excised,” Lehman said. (Related: Breast Cancer Industry A Scam? Support Education, Not Medication.)
“Our goal is to apply the tool in clinical settings to help make more informed decisions as to which patients will be surveilled and which will go on to surgery. I believe we can capitalize on machine learning to inform clinical decision making and ultimately improve patient care,” Dr. Bahl added.
This is not the first instance that AI has been used to determine the presence of cancer cells in a person. Earlier this May, Chinese startup Infervision revealed that its AI system can be used in early-stage lung cancer screening, tripling the speed at which radiologists diagnosed computerized tomography (CT) scans and decreasing the rate of missed cancer diagnoses by around 50 percent.
Read more stories such as this one at CancerCauses.news.
Sources include:
Tagged Under: artificial intelligence, biopsy, breast cancer, cancerous, high-risk breast lesions, machine learning, medical discoveries, surgical procedures